Research
‘Troublemaker’ platelet cells appear with ageing

A new study from UC Santa Cruz has found that a certain population of ‘troublemaker’ blood platelet cells appear with ageing which can lead to blood clotting. The team suggests that targeting this population of platelets could help better treat blood clotting-related diseases.
As people age, they become more prone to blood clotting diseases, when blood cells called platelets clump together when they don’t need to and can cause major issues such as strokes and cardiovascular disease. For decades, scientists have studied why older people’s blood cells behave in this way, using their insights to develop the myriad of blood-thinning drugs now on the market for treating the leading cause of death in the United States.
UC Santa Cruz Professor of Biomolecular Engineering Camilla Forsberg and her research group have now discovered a distinct, secondary population of platelets that appears with ageing and have hyperreactive behaviour and unique molecular properties, which could make them easier to target with medication.
In their paper, published in Cell, the researchers traced this population of platelets to its stem cell origins, finding what they identify as the first-ever-discovered age-specific development pathway from a stem cell to a distinct mature platelet cell.
“The question for decades and decades has been: why are aging people at such high risk for excessive blood clotting, stroke, and cardiovascular disease?” Forsberg said.
“We have this discovery of a whole new pathway that progressively appears with ageing — troublemakers. That was never part of the discussion.”
Understanding platelets
Platelet cells are one of three types of blood cells produced by the body, with red and white blood cells being the other two. Millions of these cells float around in the blood at all times, and when an injury occurs either internally or externally, they clot together to form a natural, living bandaid. Platelet dysregulation, which is known to increase with age, occurs when these cells are either hyperreactive and form clots too often, or are underperforming. In both cases the body can’t properly manage bleeding and clotting, although hyperreactivity is a much more widely-seen problem.
All blood cells begin as hematopoietic stem cells, a special class of stem cells, and then mature through a series of intermediary steps called a “differentiation pathway” that lead them to their fate as either platelets, red blood cells, or white blood cells. It’s been known for decades that these hematopoietic stem cells decline with age, but that presents a contradiction for scientists: if the hematopoietic cells are less healthy, then why are the platelets they create hyperreactive?
A ‘shortcut’ pathway
As stem cell biologists, the researchers at UC Santa Cruz approached this question by investigating the hematopoietic stem cells.
They conducted experiments that allowed them to trace the lineages of these stem cells in mouse models, and discovered that in aged mice some of their platelets did not travel along the differentiation pathway. Instead, they took what the UCSC researchers dubbed a “shortcut” pathway, skipping over the intermediary steps and immediately becoming megakaryocyte progenitors, the blood cell stage immediately before platelet production. To the researchers’ knowledge, this is the first age-specific stem cell pathway ever discovered.
“People think of [platelets and red blood cells] as one lineage that shares regulation and intermediate stages until the very end,” Forsberg said. “To see that [the secondary platelet population] were completely separated all the way from the stem cell level, only in aged mice, was really surprising.”
While the population of platelets produced from the shortcut pathway are hyperreactive, the platelets produced from the main pathway continue to behave like the platelets in a young person.
“The gradual differentiation cascade maintains a youthful property, and I feel like that is also surprising within itself,” Poscablo said.
They found that the hyperreactive secondary platelets start to be produced around midlife for the mice, with their population growing progressively with aging. As of now, the researchers have not found a trigger that begins the production of this secondary pathway. Unexpectedly, however, it does not seem to be triggered by the aging environment itself: when a young hematopoietic stem cell is transferred into an aged environment, it doesn’t seem to trigger the shortcut pathway; and when an aged hematopoietic stem cell is put into young environment, the old stem cells continue to operate as old stem cells.
“That was surprising, the age resilience of the other pathway,” Forsberg said. “One of the platelet populations is not affected at all [by aging], whereas the one we have discovered is — so the whole phenomenon is not primarily induced by the environment, but by the differentiation path.”
Choosing better treatments
Knowing that this secondary population of platelets exists will help researchers find new ways to target and regulate these problematic cells via their stem cells. Before this, researchers have not tried to target these upstream cells.
“From our expertise, we can ask the questions of how to target the hematopoietic stem cell and now the megakaryocyte progenitor, which has never really been highlighted before as a place to target,” said First author Donna Poscablo, Forsberg’s former Ph.D. student who is now a postdoctoral scholar at Stanford University.
Targeting these cells may not require the creation of new medications, but more simply inform the prescription of existing blood thinners such as Aspirin, which treat different patients to varying degrees even if they present with similar clotting-related symptoms. Using their mouse models, the researchers will identify which of the two populations of stem cells are more sensitive to Aspirin and the myriad of other platelet drugs on the market.
The UCSC researchers are also currently working on finding this secondary population of platelets in human cells with the support of a grant from the California Institute for Regenerative Medicine (CIRM). In the mouse models, they will continue to study how to manipulate and control the shortcut pathway, with funding from the National Institutes of Health (NIH) .
Collaborators on this research included UCSC Assistant Professor of Applied Mathematics Vanessa Jönsson and University of Michigan Medical School’s Reheman Adili and Michael Holinstat. Current and former IBSC scholars on this project included Atesh Worthington (now at UC San Francisco), Stephanie Smith-Berdan, Marcel Rommel, Bryce Manso, Lydia Mok, Roman Reggiardo, Taylor Cool, Raana Mogharrab, Jenna Myers, Steven Dahmen, Paloma Medina, Anna Beaudin (now at the University of Utah, Salt Lake City), and Scott Boyer.
Research
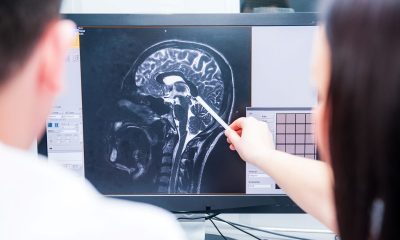
NHS to review cost effectiveness of new Alzheimer’s drugs

NICE will review whether new Alzheimer’s drugs should be offered on the NHS after an appeal found their wider impact was not fully counted.
An appeal found that the National Institute for Health and Care Excellence had failed to properly account for the wider impact of the treatments, including the heavy burden on unpaid carers, when calculating the cost effectiveness of the medicines.
Both treatments, lecanemab and donanemab, will now return to a NICE committee for further consideration.
“Today’s ruling is an opportunity for NICE to consider the real cost of Alzheimer’s on people and their families, and we welcome the decision to look again at whether new medicines could be provided on the NHS,” said David Thomas, head of policy and public affairs at Alzheimer’s Research UK.
Lecanemab and donanemab do not cure Alzheimer’s, but they slow it by targeting and clearing clumps of amyloid proteins, sticky protein build-ups in the brain linked to the disease.
While the drugs are available privately in the UK for people who can afford them, NICE ruled last year that they were too expensive to be made available on the NHS in England and Wales.
It is estimated informal dementia care costs the economy more than £20bn a year.
Alzheimer’s Research UK wants NICE to update how it assesses the value of new dementia drugs and factor in the huge additional costs this condition places on society and the wider economy.
NICE and its expert committees assess whether new drugs are good value for money for the NHS based on a wide range of evidence.
This includes how treatments perform in clinical trials, the experiences of patients and carers, and the costs of new drugs as well as any changes to NHS services needed to provide access.
When NICE weighs up whether a new Alzheimer’s drug is cost effective for the NHS, it carries out a limited assessment of the impact dementia has on the health of carers.
But the condition takes an enormous toll on families and society because caring for someone with dementia can lead people to become more isolated and give up work.
It can have a major emotional impact and put families under financial strain.
Thomas said: “Research has delivered new treatments with the potential to provide people with valuable extra months of independence, lessening the burden on carers.
“While these treatments offer modest benefits and can cause serious side effects, they provide the foundation for a future where dementia becomes a treatable condition.
“Now we need NICE to look again at how these medicines could benefit both people with early Alzheimer’s and their carers.”
Chris, whose mother Shirley is living with Alzheimer’s disease, said: “The real cost of Alzheimer’s is far greater than many people realise.
“In order to give my mum the care she needed, I moved back home to help my dad as the care was too much for him alone. After my dad passed away from Covid in 2021, I became sole carer for my mum.
“It was a very difficult period, working a full-time job, caring for Mum and dealing with the loss of my dad. Eventually I got some in-home care support to help.
“The family has borne most of the cost of Mum’s care, both in time and fees, and the family home has been sold to finance it.”
“The emotional and financial strain Alzheimer’s has taken on our family is horrendous, and I know many families across the UK are experiencing this pressure.”
He is backing Alzheimer’s Research UK’s call for NICE to change how it evaluates new dementia treatments.
The timeframe for the next NICE meetings to discuss the drugs is still to be set, and it is not certain follow-up hearings would change NICE’s guidance on access to the medicines.
But Alzheimer’s Research UK is continuing to push to make sure dementia is now a main priority for political and NHS decision-makers.
The head of the ongoing independent review into adult social care, Baroness Louise Casey, has called on the government to act, show leadership and prioritise dementia.
She has proposed appointing a dementia tsar to drive forward the prevention, treatment and care of dementia.
Baroness Casey has also argued for more funding for dementia treatment trials.
With more than 130 Alzheimer’s drugs in clinical trials worldwide, the charity says it is vital the NHS runs trials of new treatments now to understand how to deliver them to eligible patients in future.
In addition to changing how NICE assesses new medicines, the health service needs to collect real-world evidence on new dementia drugs and prepare for diagnostic tests and innovative treatments that are coming.
“Alzheimer’s Research UK is calling on the government to give dementia the same political determination that transformed cancer care,” Thomas said.
“We urgently need investment and a clear UK-wide plan so new treatments can be assessed in the NHS and reach the people who stand to benefit.”
Health and social care secretary Wes Streeting has said dementia is “one of the greatest challenges of our time” and pledged that the UK should become a world leader in dementia clinical trials.
News
Osteoporosis drugs could reduce dementia risk, study suggests
News
Gut health supplement relieves arthritis pain, research finds

A prebiotic fibre supplement may ease arthritis pain and improve grip strength in people with knee osteoarthritis, a study suggests.
The daily supplement, made from inulin, a dietary fibre found in chicory root, Jerusalem artichokes and other vegetables, also lowered pain sensitivity and saw fewer people drop out than a digital physiotherapy programme tested alongside it.
Dr Afroditi Kouraki, lead author of the study from the University of Nottingham, said: ‘Our findings suggest that targeting gut health with a prebiotic supplement is a safe, well-tolerated, and effective way to reduce pain in people with knee osteoarthritis.
“The very low dropout rate compared to the exercise group is also encouraging from a public health perspective, people were able to fit this supplement easily into their daily lives.’
Osteoarthritis of the knee, a wear-and-tear joint condition, affects hundreds of millions of people worldwide and is a leading cause of pain and disability, particularly in older adults.
Current treatments rely heavily on pain medication, which can cause side effects, or exercise programmes, which many patients find hard to maintain.
The INSPIRE trial, led by researchers at the University of Nottingham, involved 117 adults with knee osteoarthritis and tested four groups: inulin alone, digital physiotherapy-supported exercise alone, a combination of both, and a placebo. Both inulin and physiotherapy independently reduced knee pain.
However, inulin alone improved grip strength and reduced pain sensitivity, measures linked to how the nervous system processes pain, while physiotherapy did not.
The dropout rate for those taking the supplement was just 3.6 per cent, compared with 21 per cent for the physiotherapy group, suggesting a daily supplement may be easier for people to stick with than an exercise programme.
Inulin works as a prebiotic, meaning it feeds beneficial bacteria in the gut.
This leads to the production of compounds called short-chain fatty acids, particularly butyrate, which can affect inflammation and pain pathways throughout the body.
Participants taking inulin also showed increased levels of both butyrate and GLP-1, a gut hormone linked to pain regulation and muscle health.
Higher GLP-1 levels were associated with improved grip strength, pointing to a possible gut-muscle connection.
Senior author Professor Ana Valdes added: ‘The link we observed between GLP-1 and grip strength is particularly intriguing and points to a broader gut-muscle-pain axis that warrants further investigation. This could have implications not just for osteoarthritis, but for understanding how gut health influences ageing and physical resilience more broadly.’
Professor Lucy Donaldson, director of research at Arthritis UK, said: “The pain of arthritis can severely impact quality of life. Our recent lived experience survey showed that six in ten people are living in pain most or all of the time due to their arthritis.
“Researchers are starting to explore the role of the gut microbiome in our experience of pain.
“This exciting preliminary research highlights how diet and physiotherapy can act in different ways to have benefits for people with arthritis.
“We know a variety and balance of healthy foods, including fibre, and regular physical activity matter, and we’re glad to be supporting research that explores how they work to help people with arthritis.”