Wellness
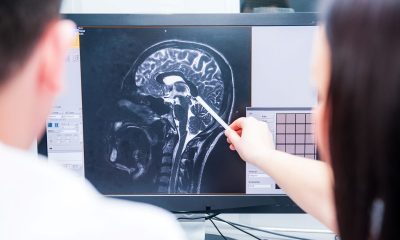
Brain stimulation effectiveness tied to learning ability, not age

As we age, our cognitive and motor functions deteriorate, which in turn affects our independence and overall quality of life. Research efforts to ameliorate or even completely abolish this have given rise to technologies that show a lot of promise.
Among these is non-invasive brain stimulation: a term encompassing a set of techniques that can affect brain functions externally and noninvasively, without the need for surgery or implants.
One such promising technique, in particular, is anodal transcranial direct current stimulation (atDCS), which uses a constant, low electrical current delivered via electrodes on the scalp to modulate neuronal activity.
However, studies exploring atDCS have produced inconsistent results, which has prompted researchers to explore why some people benefit from atDCS while others don’t.
The problem seems to lie in our understanding of factors that may influence responsiveness to brain stimulation, leading to responders and non-responders; among these, age has been suggested as one important factor.
Some studies suggest further factors such as baseline behavioural abilities and previous training might be important considerations, but an interplay of these factors with behaviour has not been determined in detail, pointing to the need of refined predictive models of the effects of atDCS.
Now, scientists led have identified an important factor affecting an individual’s responsiveness to atDCS.
The team looked at how native learning abilities determine the effect of brain stimulation applied while learning a motor task. Their findings suggests that individuals with less efficient learning mechanisms benefit more from stimulation, while those with optimal learning strategies might experience negative effects.
The researchers recruited 40 participants: 20 middle-aged adults (50 to 65 years old) and 20 older adults (over 65). Each group was further divided into those receiving active atDCS and those receiving placebo stimulation.
Over ten days, participants practiced a finger-tapping task designed to study motor sequence learning at home while receiving atDCS. The task involved replicating a numerical sequence using a keypad, trying to be as fast and as accurate as possible.
The team then used a machine-learning model trained on a public dataset to classify participants as either “optimal” or “suboptimal” learners, based on their initial performance. This model aimed to predict who would benefit from atDCS, based on their ability to integrate information about the task efficiently early during training
The study found that suboptimal learners, who were seemingly less efficient at internalising the task at the early stages of learning, experienced an accelerated accuracy improvement while performing the task when receiving atDCS. This effect was not limited to people of a certain age (e.g., older adults), with suboptimal learners being found among younger individuals as well.
In contrast, participants with optimal learning strategies, regardless of age, even showed a negative trend in performance when receiving atDCS.
This difference suggests that brain stimulation is more beneficial for individuals who initially struggle with motor tasks. As such, atDCS seems to possess a restorative rather than an enhancing quality, with important implications for rehabilitation.
“By leveraging different methods in Machine learning, we were able to untangle the influence of different factors on the individual effects of brain stimulation,” says Pablo Maceira, the study’s first author.
“This will pave the way to maximize the effects of brain stimulation in individual subjects and patients.”
The study implies that, in the long run, personalised brain stimulation protocols will be developed to maximize benefits based on an individual’s specific needs, rather than a common trait such as age.
This approach could lead to more effective brain stimulation-based interventions, targeting specific mechanisms supporting learning, especially in the view of neurorehabilitation, for which the main basis is the re-learning of lost skills due to a brain lesion (e.g., after a stroke or a traumatic brain injury).
“In the future, clinicians could apply a more advanced version of our algorithm to determine whether a patient will benefit from a brain stimulation-based therapy, to enhance the effects of neurorehabilitation and personalize treatment,” says Friedhelm Hummel at EPFL.
Wellness
Gut-friendly foods may damage heart, charity warns
News
Diabetes patients face increased risk of undiagnosed heart failure

People with diabetes may have undiagnosed heart failure that could be detected by a simple screening blood test, research suggests.
The TARTAN-HF trial found that one in four patients with diabetes who had at least one other risk factor for heart failure had undiagnosed heart failure detected through screening with a blood test and ultrasound scanning of the heart.
Experts said the findings show the extent of unrecognised heart failure in people with diabetes, and how the condition can be detected using a widely available blood test called NT-proBNP, which measures how much strain the heart is under.
They suggest a heart failure screening programme for diabetics could improve diagnosis rates, lead to earlier treatment and potentially reduce the risk of hospitalisation and death.
The study, involving 700 patients, was led by the University of Glasgow in collaboration with AstraZeneca, Roche Diagnostics, Us2.ai, NHS Greater Glasgow and Clyde and NHS Lanarkshire.
Dr Kieran Docherty, clinical senior lecturer at the University of Glasgow’s School of Cardiovascular and Metabolic Health, said: “Our results from the landmark TARTAN-HF trial identified heart failure in a large proportion of people living with diabetes, emphasising the need for a heart failure screening strategy in this group of patients.
“We know that many of the symptoms and signs of heart failure are non-specific, and may go unrecognised as potentially being due to heart failure for a long time.
“The strategy used in our trial is simple and easy to implement in clinical practice, and will aid in the early identification of heart failure in people with diabetes, and facilitate the initiation of medications that we know improve outcomes in patients with heart failure.”
The study, which began more than three years ago, involved more than 700 people with diabetes from the two health board areas who had at least one other risk factor for heart failure.
They were randomly assigned either to receive heart failure screening or to continue with their usual care.
Researchers found screening uncovered a large number of previously unrecognised cases of heart failure. Around one in four, or 24.9 per cent, of those screened were found to have the condition within six months, compared with 1 per cent in the group continuing their usual care.
The study, involving patients with type 1 and type 2 diabetes, found almost all of the participants found to have heart failure had preserved ejection fraction, which can be difficult to detect without dedicated testing.
The findings of the TARTAN-HF trial were presented at the American College of Cardiology conference taking place from 28 to 30 March in New Orleans in the US.
Dr Edward Piper, medical director at AstraZeneca UK, said: “Delayed diagnosis and treatment of heart failure in people with type 2 diabetes contributes to poor long-term outcomes. TARTAN-HF demonstrates that targeted, risk-based screening can identify previously undiagnosed heart failure in approximately one in four high-risk patients with diabetes, enabling earlier intervention with guideline-directed therapy.”
Dr Christian Simon, head of global medical affairs at Roche Diagnostics, said: “We are proud to have supported the landmark TARTAN-HF trial. These findings demonstrate the transformative power of early, accessible diagnostics like the NT-proBNP blood test.
“By identifying unrecognised heart failure in people with diabetes, we enable clinicians to initiate appropriate treatments sooner, ultimately improving patient outcomes and lives.”
News
UK government announces £6.3m fund to boost men’s health

The UK has launched a £6.3m men’s health fund to back local projects aimed at helping men and boys live longer, healthier lives.
The Men’s Health Community Fund is a partnership between the Department of Health and Social Care, Movember and People’s Health Trust.
The government is contributing £3m, while the two charities are more than doubling that to take the total to £6.3m.
Grants will support community projects reaching underserved men and boys aged 16 and over, particularly in the most disadvantaged areas and at key points in their lives such as becoming a father, losing a job or retiring.
Projects could include support for new fathers, activities for men facing loneliness and social isolation, services to help young men engage with the health system, and support for men in work, out of work and moving into retirement.
The programme will bring together voluntary, community and social enterprise organisations to test new ways of reaching men who are least likely to use traditional health services.
An evaluation funded through the National Institute for Health and Care Research will assess what works and help inform future policy and delivery.
Health and social care secretary Wes Streeting said: “Too many men across the country are living shorter, less healthy lives, particularly those in our most disadvantaged communities.
“This new partnership will help men get the support they need in the places they feel most comfortable, their communities, among people they trust.
“By working with expert charities and local organisations, we can reach the men who are too often missed by traditional services and help them take better care of their mental and physical health.”
“It is a key step in delivering our first ever Men’s Health Strategy and driving forward our ambition to halve the gap in healthy life expectancy between the richest and poorest areas.”
The Men’s Health Strategy sets out plans to tackle the physical and mental health challenges men and boys face.
Men can be less likely to seek help and more likely to suffer in silence, while higher rates of smoking, drinking, gambling and drug use are damaging men’s health and affecting families, workplaces and communities.
The government is also investing £3.6m over the next three years in suicide prevention projects for middle-aged men in local communities across areas of England where men are most at risk, many of which are also among the most deprived. Suicide is one of the biggest killers of men under 50, and three-quarters of all suicides are men.
The projects will aim to break down barriers middle-aged men face in seeking support, including stigma around asking for help and a lack of awareness of what is available and how to access it.
They will be co-designed with experts and men with lived experience of mental health crises and suicidal thoughts.