News
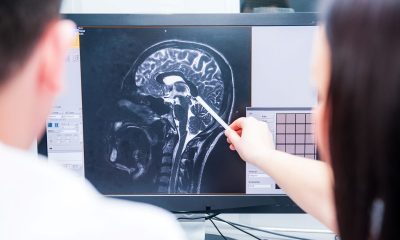
New research shows it’s never too late to tackle alcohol abuse

It’s no secret that our planet is ageing – and not just in terms of the physical entity we live on.
The world is facing a demographic timebomb with the scales tipped firmly toward older adults.
Global life expectancy a century ago was just 34 years. Now, thanks to medical advances and improved standards of living, the average life span has soared to 72 years.
As the last of the baby boomer generation born between the end of the Second World War and the mid-1960s move into their retirement years, the number of older people is expected to significantly outnumber children under the age of 10 by 2030 – 1.41bn versus 1.35bn – according to the United Nations.
Projections indicate that by 2050 those aged 60-plus will account for 2.1bn of the world’s population compared to just two billion adolescents and youths aged 10-24.
Good as it is that we all have the potential to live longer, it brings with it a host of problems, not least on the healthcare front. One challenge facing healthcare professionals is the rising rates of alcohol use in older adults.
Drinking too much can have an adverse physical and mental impact on anyone of any age, whether it be mood swings, heart and liver problems, or an increased risk of cancer. But age-related changes in the body put older adults at heightened risk as they typically metabolise alcohol less quickly and feel its effects more keenly than younger people do.
This – coupled with the fact many older adults are taking a cocktail of prescription medicines that often don’t mix well with alcohol with sometimes dangerous and even fatal consequences – is much cause for concern.

Jeppe Tryggedsson
Often, however, health professionals are loath to persuade older people to seek help with their alcohol abuse due “to a misguided notion that alcohol might be the last thing providing them with a quality of life,” Jeppe Tryggedsson, a PhD student at the University of Southern Denmark, told Agetech World.
But a new study from UCAR – the Unit for Clinical Alcohol Research at the University of Southern Denmark – suggests that even a modest reduction in alcohol consumption and participation in a treatment programme can make a significant difference for individuals aged 60-plus with a notable liquor intake.
The research has shown that older adults undergoing treatment experience an improved quality of life, whether they choose to abstain from alcohol entirely or reduce their consumption.
Now Tryggedsson, a candidate in public health science and lead author of the study, hopes the work carried out by him and his colleagues, will dispel the myth that older adults with alcohol use disorder, don’t necessarily need treatment.
Speaking to Agetech World, he said it had been noted that individuals who completely abstain from drinking and those who reduce their intake both experienced improvements in quality of life.
This improvement extended across all domains – mental, physical, social, and environmental.
He explained: “In our study, the quality of life of older adults suffering from alcohol use disorder does not decline following treatment. On the contrary, it improves, at least slightly, both overall and within various domains.
“These improvements are not only maintained over time but also keep increasing up to one year after initiating treatment. Thus, quality of life measures is still significantly greater one year after treatment entry compared to baseline measures.
“We were also able to show that these improvements might also be achievable in patients with a reduction goal as a treatment outcome, and not only for patients who obtain abstinence after treatment.
“This knowledge is highly relevant for healthcare professionals who tend to believe that either there is no perspective in offering treatment for older adults late in life or that alcohol reduction is not a feasible goal for the older adults who aim for it.”
Tryggedsson said addressing this reluctance among healthcare professionals was particularly important, “since it is probably a part of the explanation of why older adults are less likely to receive treatment compared to other age groups.
“Overall, our results indicate that it would be highly beneficial to convert this attitude of reluctance to treat older adults for their excessive alcohol use and further improve treatment options for older populations.
“Furthermore, it may also be relevant to continuously convey to patients that improvements in quality of life continue over time, to help prevent a feeling of hopelessness.
“It is my overall hope that more people with problematic alcohol use will use this knowledge to seek treatment.
“Hopefully, our study will encourage individuals, family members, and peers, to believe that there are feasible alternatives to drinking late in life, regardless of age and gender.”
The researchers used data from the Elderly Study, a multinational, randomised controlled clinical trial conducted between January 2014 and May 2016.
The study was conducted in six treatment institutions in three countries – Denmark (Copenhagen, Aarhus, and Odense), Germany (Munich and Dresden), and the United States (Albuquerque, New Mexico) – and consisted of 693 patients aged 60 or older.
Patients underwent treatment for alcohol use disorder through a conversation-based rehabilitation method called motivational enhancement therapy aimed at boosting enthusiasm levels for behaviour change and promoting engagement in the process.
The patients completed questionnaires at the beginning of treatment and were followed up at four and 12 weeks, six months and a year.
Information on sociodemographic factors, alcohol consumption, quality of life, and more was collected during the follow-ups.
Tryggedsson said: “At times, achieving complete abstinence isn’t realistic, especially for patients dependent on alcohol. Even starting from a high point, a reduction yields a significant effect. Both the treatment process and the post-treatment period are pivotal.”
He believes the results can serve to enlighten therapists and physicians, highlighting the importance of encouraging older adults with alcohol use disorder to seek treatment.
“When they observe signs of alcohol-related issues in patients, they should address it without hesitation and confront potential abuse. In doing so, they are providing a valuable service to the patients, even if the patients may not recognise it as such,” Tryggedsson stated.
For decades the public has been confronted with conflicting research-led advice when it comes to alcohol intake. Too much alcohol is bad for you; a little does you no harm; red wine is better than white; the occasional binge will help keep your spirits up (no pun intended).
But in January 2023, the World Health Organisation published a statement in The Lancet Public Health saying that when it comes to alcohol consumption, there is no safe amount that doesn’t affect health.
Much of the focus has been on trying to encourage young people to avoid alcohol, however, with little effort directed at the older age group. It was this that Tryggedsson said first encouraged him to conduct a study specifically aimed at older adults and alcohol abuse.
“In Denmark, there is a lot of focus on the problematic alcohol use in our younger age groups. It is often said that Danish young people, down to 15-year-olds, are the European champions of being intoxicated and binge drinking. A record you can’t be very proud of from a public health perspective,” he expounded.
“There are lots of reasons to focus on problematic alcohol use during childhood and adolescence – binge drinking being one of them. However, when looking into which age groups exceed Danish National guidelines of no more than 10 drinks per week, the highest proportions are seen within men aged 65-74 years old (32.5%).
“Among men, two other age groups exceed the proportion seen among the 16-24 year-olds (23.9%), that is the 55-64 year-olds and the plus 75 year olds (27.1% and 29.9%, respectively).
“Among women, the highest proportions are seen among the 16-24 year-olds and the 65-74 year-olds (14.0% and 13.7%, respectively).
“Thus, older Danish adults, especially men, make up the largest proportion of people who exceed Danish National guidelines of no more than 10 drinks per week.
“Furthermore, these numbers are not decreasing over time at the same rate in the older age groups as among the younger ones.
“As my colleagues had recently performed a study, comparing two psychosocial interventions aimed at treating alcohol use disorder in older adults (60-plus years), I was able to use their data to investigate gender differences in an older population of alcohol use disorder patients, an area of interest that arose when looking at the Danish numbers.”
Most noticeable were gender differences in drinking patterns, which seemed to be particularly pronounced among older adults. Tryggedsson said: “Older men are reported to drink more often and in higher quantities than older women, resulting in higher rates of hospitalisation and more deaths in men.
“Furthermore, binge drinking, which leads to the greatest level of harm, is much more frequent among older men than women. Overall, it is estimated that the number of older adults suffering from AUD is higher in men than in women.”
But Tryggedsson noted: “In recent years, however, the gender gap in alcohol use has been reduced, mainly due to older women drinking more often and in higher quantities, including binge drinking.”
There are several reasons as to why gender differences exist in alcohol use, especially in older populations, Tryggedsson told Agetech World. “Older adults may experience widowhood, living alone, retirement, and a dwindling social network. Specifically, older women have been found to be more frequently widowed, living alone, and showing higher rates of retirement compared to older men. Thus, gender potentially interacts with other factors, and often with several at a time.”
Given his study has shown that older adults dealing with alcohol use disorder can be helped towards a better quality of life, why does Tryggedsson think that within the medical profession helping this age group has traditionally been seen as a ‘lost cause.’
“There are several possible reasons for this. Older adults may be less likely to disclose a history of excessive alcohol use. Also, the presentation of excessive alcohol use in older adults may be atypical, such as falls, confusion, and depression, and masked by comorbid physical or psychiatric illness, which makes detection all the more difficult.
“Thus, healthcare workers might have a lower degree of suspicion when assessing older people. Healthcare workers may also perceive alcohol use disorders in older people as being understandable in the context of poor health and changing life circumstances.
“Lastly, national guidelines on alcohol consumption may not apply to older people because of age-related changes in metabolism, advancing ill health, and increased sensitivity to the effects of alcohol.
“All of these factors are likely to result in under-detection and misdiagnosis of alcohol use disorder in older adults, among other things, by giving false impressions of the true extent of the problem.”
News
Gut-friendly foods may damage heart, charity warns
Wellness
Diabetes patients face increased risk of undiagnosed heart failure

People with diabetes may have undiagnosed heart failure that could be detected by a simple screening blood test, research suggests.
The TARTAN-HF trial found that one in four patients with diabetes who had at least one other risk factor for heart failure had undiagnosed heart failure detected through screening with a blood test and ultrasound scanning of the heart.
Experts said the findings show the extent of unrecognised heart failure in people with diabetes, and how the condition can be detected using a widely available blood test called NT-proBNP, which measures how much strain the heart is under.
They suggest a heart failure screening programme for diabetics could improve diagnosis rates, lead to earlier treatment and potentially reduce the risk of hospitalisation and death.
The study, involving 700 patients, was led by the University of Glasgow in collaboration with AstraZeneca, Roche Diagnostics, Us2.ai, NHS Greater Glasgow and Clyde and NHS Lanarkshire.
Dr Kieran Docherty, clinical senior lecturer at the University of Glasgow’s School of Cardiovascular and Metabolic Health, said: “Our results from the landmark TARTAN-HF trial identified heart failure in a large proportion of people living with diabetes, emphasising the need for a heart failure screening strategy in this group of patients.
“We know that many of the symptoms and signs of heart failure are non-specific, and may go unrecognised as potentially being due to heart failure for a long time.
“The strategy used in our trial is simple and easy to implement in clinical practice, and will aid in the early identification of heart failure in people with diabetes, and facilitate the initiation of medications that we know improve outcomes in patients with heart failure.”
The study, which began more than three years ago, involved more than 700 people with diabetes from the two health board areas who had at least one other risk factor for heart failure.
They were randomly assigned either to receive heart failure screening or to continue with their usual care.
Researchers found screening uncovered a large number of previously unrecognised cases of heart failure. Around one in four, or 24.9 per cent, of those screened were found to have the condition within six months, compared with 1 per cent in the group continuing their usual care.
The study, involving patients with type 1 and type 2 diabetes, found almost all of the participants found to have heart failure had preserved ejection fraction, which can be difficult to detect without dedicated testing.
The findings of the TARTAN-HF trial were presented at the American College of Cardiology conference taking place from 28 to 30 March in New Orleans in the US.
Dr Edward Piper, medical director at AstraZeneca UK, said: “Delayed diagnosis and treatment of heart failure in people with type 2 diabetes contributes to poor long-term outcomes. TARTAN-HF demonstrates that targeted, risk-based screening can identify previously undiagnosed heart failure in approximately one in four high-risk patients with diabetes, enabling earlier intervention with guideline-directed therapy.”
Dr Christian Simon, head of global medical affairs at Roche Diagnostics, said: “We are proud to have supported the landmark TARTAN-HF trial. These findings demonstrate the transformative power of early, accessible diagnostics like the NT-proBNP blood test.
“By identifying unrecognised heart failure in people with diabetes, we enable clinicians to initiate appropriate treatments sooner, ultimately improving patient outcomes and lives.”
News
UK government announces £6.3m fund to boost men’s health

The UK has launched a £6.3m men’s health fund to back local projects aimed at helping men and boys live longer, healthier lives.
The Men’s Health Community Fund is a partnership between the Department of Health and Social Care, Movember and People’s Health Trust.
The government is contributing £3m, while the two charities are more than doubling that to take the total to £6.3m.
Grants will support community projects reaching underserved men and boys aged 16 and over, particularly in the most disadvantaged areas and at key points in their lives such as becoming a father, losing a job or retiring.
Projects could include support for new fathers, activities for men facing loneliness and social isolation, services to help young men engage with the health system, and support for men in work, out of work and moving into retirement.
The programme will bring together voluntary, community and social enterprise organisations to test new ways of reaching men who are least likely to use traditional health services.
An evaluation funded through the National Institute for Health and Care Research will assess what works and help inform future policy and delivery.
Health and social care secretary Wes Streeting said: “Too many men across the country are living shorter, less healthy lives, particularly those in our most disadvantaged communities.
“This new partnership will help men get the support they need in the places they feel most comfortable, their communities, among people they trust.
“By working with expert charities and local organisations, we can reach the men who are too often missed by traditional services and help them take better care of their mental and physical health.”
“It is a key step in delivering our first ever Men’s Health Strategy and driving forward our ambition to halve the gap in healthy life expectancy between the richest and poorest areas.”
The Men’s Health Strategy sets out plans to tackle the physical and mental health challenges men and boys face.
Men can be less likely to seek help and more likely to suffer in silence, while higher rates of smoking, drinking, gambling and drug use are damaging men’s health and affecting families, workplaces and communities.
The government is also investing £3.6m over the next three years in suicide prevention projects for middle-aged men in local communities across areas of England where men are most at risk, many of which are also among the most deprived. Suicide is one of the biggest killers of men under 50, and three-quarters of all suicides are men.
The projects will aim to break down barriers middle-aged men face in seeking support, including stigma around asking for help and a lack of awareness of what is available and how to access it.
They will be co-designed with experts and men with lived experience of mental health crises and suicidal thoughts.