News
Have scientists finally found the cure for ageing?

Cleopatra is said to have favoured asses’ milk, the ancient Greeks olive oil and yoghurt, Elizabethan women slices of raw meat, the Georgians mature wine, and the Victorians honey, oatmeal and egg yolks.
The above may read like a catalogue of fashionable foods from an historical grocery list or the latest fad diet. But in their day these mixed bag of ingredients were considered to be cutting-edge anti-ageing cures.
The fight against wrinkles and lines has been preoccupying humans if not quite from the dawn of time, from at least 2500BC when the people of the Indus Valley Civilisation are known to have developed powders and herbal remedies to improve not just their complexion but prevent thinning tresses and the appearance of grey hair.
The desire to turn back the human biological clock and stay forever young has become the modern day Holy Grail. According to industry research company IMARC Group, the global anti-ageing market was worth US $67.2bn in 2022. That figure is predicted to swell to a staggering US $98.6bn by 2028 on the back of a rising awareness of the plethora of anti-ageing products now on the market, the increased consciousness among individuals about their physical appearance, and the growing popularity of non-surgical procedures and treatments designed to counter the process of becoming old.
Reversing or slowing down the effects of ageing isn’t just pre-occupying the beauty industry and the billions around the world slavishly buying into medical procedures and over-the-counter remedies promising to restore a youthful body and complexion.
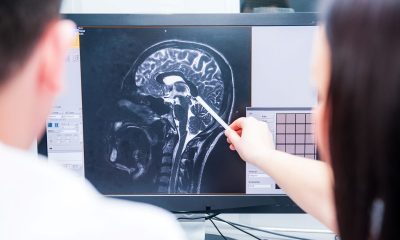
Research scientists too are captivated with finding an answer to the centuries old question of how the brakes can be applied to ageing.
And not necessarily for the sake of our vanity. Ageing is the most debilitating problem humans face. Sadly, getting old can open a Pandora’s box of unpleasant health issues, from cancer to dementia, mobility problems, hearing loss, diabetes, pulmonary disease and depression.
According to the latest figures from the EU, 84.9% of all deaths in 2020 across European Union countries occurred in people over the age of 65. Of those, just over a third (35%) of deaths were caused by diseases of the circulatory system. Nearly one in three of these (11%) were as a result of ischaemic heart disease.
The second most common cause of death among elderly people was cancer at 20.5%.
But a growing number of scientists claim it doesn’t have to be like this and are seeking ways of rebooting the body.
According to João Pedro de Magalhães, a professor of Molecular Biogerontology in the Institute of Inflammation and Ageing at the University of Birmingham in the UK, most mechanistic explanations of ageing put forward that it’s caused by the accumulation of one or more forms of molecular damage.
But Professor Magalhães thinks otherwise. He believes ageing could be seen as an error in the software that guides how our bodies regulate themselves. In other words, ageing is a software design flaw, and to understand the process scientists need to decode human genetic software.
Professor Magalhães has been exploring the question of why ageing happens uniformly, when current models work on the assumption that we accumulate ‘damage’ randomly, and has recently had a review published on the subject in the open access scientific journal, Genome Biology.
“If we imagine that the human body is a bit like a computer, the paper suggests that ageing is not an accumulation of damage to the hardware, but a process driven by design flaws in the software, a radical departure from damage-based theories that until now have prevailed in ageing research,” he explained.
“Ageing is inherent to all human beings. It is widely thought that ageing occurs due to the accumulation of various forms of molecular damage. What if, however, ageing changes are not primarily a result of a build-up of stochastic, random damage but are rather a product of regulated processes?
“In other words, what if we age not because of inevitable damage to the hardware but rather because of the software, defined as the DNA code that orchestrates how a single cell develops into an adult organism? As a result, we could see ageing is an information problem.”
He suggests that medical interventions to combat ageing could be based on a faulty premise and needs to be reconsidered in light of the uniform, DNA-encoded nature of ageing.
Professor Magalhães compares the challenge of understanding ageing to how a computer system functions, likening cells and their components to computer hardware, and genetic information to software.
He argues that interventions akin to a computer restart, such as cell reprogramming, which is also known as epigenetic rejuvenation, could hold clues for future interventions to promote healthy ageing.
In addition, Professor Magalhães warns that existing treatments which work on the basis that ageing is an accumulation of cell damage over time, are unlikely to lead to broad positive impacts.
He said: “Seeing ageing as the outcome of ‘flaws’ in our software has important implications for studying and developing interventions for ageing. Traditional anti-ageing interventions targeting damage, like oxidative damage and telomere shortening, will have limited success.
“By contrast, ageing therapies will only be effective if targeting the software rather than the hardware. Seeing ageing as a programmed process would transform our perception of the ageing process with multiple and profound implications.”
Professor Magalhães believes understanding the biology of ageing would shed important light on the cause of age-related diseases. He said: “I suggest that design flaws in the developmental software program contribute to the development of many age-related diseases. Even cancer, which is largely due to molecular damage, is influenced by ageing processes.”
Professor Magalhães is not alone in his thinking. A 13-year study by researchers at Harvard University has also shown that the modification of gene expression can lead to cell ageing.
The study, published in the journal Cell, suggests it is the way DNA is governed that drives ageing.
Put simply. the Harvard study is suggesting that ageing doesn’t mean that cells are damaged and incapable of behaving like young cells, but that something has got lost in translation in their genetic make-up.
The researchers say that in theory, if epigenetic (the study of stable changes in cell function that do not involve alterations in the DNA sequence) interventions are used to get cells back on the right track, they can ‘remember’ how to be young and fully functioning again, effectively reversing the ageing process.
In the main experiment using mice, the scientists at Harvard mimicked breaks in chromosomes that cells experience every day in response to things such as breathing, exposure to sunlight and contact with certain chemicals.
They ensured these breaks did not occur in the coding regions of the DNA so mutations were prevented from occurring over time. The team noticed that the epigenome grew disorganised leading to more aged looks and behaviour.
Next, they delivered gene therapy to reverse the changes and found the organs and tissues had resumed their youthful state.
The paper’s senior author, David Sinclair, a professor of genetics in the Blavatnik Institute at Harvard Medical School and co-director of the Paul F Glenn Center for Biology of Aging Research, said: “It’s like rebooting a malfunctioning computer,” explaining that the therapy “set in motion an epigenetic programme that led cells to restore the epigenetic information they had when they were young. It’s a permanent reset.”
Dr Sinclair hopes the work inspires other scientists to study how to control ageing to prevent and eliminate age-related diseases and conditions in humans, such as cardiovascular disease, type 2 diabetes, neurodegeneration, and frailty.
“These are all manifestations of ageing that we’ve been trying to treat with medicines when they arise, which is almost too late,” he said.
Co-first author Jae-Hyun Yang, a research fellow in genetics in the Sinclair lab. added: “We expect the findings will transform the way we view the process of ageing and the way we approach the treatment of diseases associated with ageing,”
The ultimate goal, Dr Sinclair concluded, would be to address the root causes of ageing to extend human health span: the number of years that a person remains not just alive, but well.
Medical applications are a long way off and will take extensive experiments in multiple cell and animal models. But, Dr Sinclair said, scientists should think big and keep trying to achieve such dreams.
“We hope these results are seen as a turning point in our ability to control aging,” said Dr Sinclair. “This is the first study showing that we can have precise control of the biological age of a complex animal; that we can drive it forwards and backwards at will.
“We’re talking about taking someone who’s old or sick and making their whole body or a specific organ young again, so the disease goes away. It’s a big idea.”
News
Gut-friendly foods may damage heart, charity warns
News
Diabetes patients face increased risk of undiagnosed heart failure

People with diabetes may have undiagnosed heart failure that could be detected by a simple screening blood test, research suggests.
The TARTAN-HF trial found that one in four patients with diabetes who had at least one other risk factor for heart failure had undiagnosed heart failure detected through screening with a blood test and ultrasound scanning of the heart.
Experts said the findings show the extent of unrecognised heart failure in people with diabetes, and how the condition can be detected using a widely available blood test called NT-proBNP, which measures how much strain the heart is under.
They suggest a heart failure screening programme for diabetics could improve diagnosis rates, lead to earlier treatment and potentially reduce the risk of hospitalisation and death.
The study, involving 700 patients, was led by the University of Glasgow in collaboration with AstraZeneca, Roche Diagnostics, Us2.ai, NHS Greater Glasgow and Clyde and NHS Lanarkshire.
Dr Kieran Docherty, clinical senior lecturer at the University of Glasgow’s School of Cardiovascular and Metabolic Health, said: “Our results from the landmark TARTAN-HF trial identified heart failure in a large proportion of people living with diabetes, emphasising the need for a heart failure screening strategy in this group of patients.
“We know that many of the symptoms and signs of heart failure are non-specific, and may go unrecognised as potentially being due to heart failure for a long time.
“The strategy used in our trial is simple and easy to implement in clinical practice, and will aid in the early identification of heart failure in people with diabetes, and facilitate the initiation of medications that we know improve outcomes in patients with heart failure.”
The study, which began more than three years ago, involved more than 700 people with diabetes from the two health board areas who had at least one other risk factor for heart failure.
They were randomly assigned either to receive heart failure screening or to continue with their usual care.
Researchers found screening uncovered a large number of previously unrecognised cases of heart failure. Around one in four, or 24.9 per cent, of those screened were found to have the condition within six months, compared with 1 per cent in the group continuing their usual care.
The study, involving patients with type 1 and type 2 diabetes, found almost all of the participants found to have heart failure had preserved ejection fraction, which can be difficult to detect without dedicated testing.
The findings of the TARTAN-HF trial were presented at the American College of Cardiology conference taking place from 28 to 30 March in New Orleans in the US.
Dr Edward Piper, medical director at AstraZeneca UK, said: “Delayed diagnosis and treatment of heart failure in people with type 2 diabetes contributes to poor long-term outcomes. TARTAN-HF demonstrates that targeted, risk-based screening can identify previously undiagnosed heart failure in approximately one in four high-risk patients with diabetes, enabling earlier intervention with guideline-directed therapy.”
Dr Christian Simon, head of global medical affairs at Roche Diagnostics, said: “We are proud to have supported the landmark TARTAN-HF trial. These findings demonstrate the transformative power of early, accessible diagnostics like the NT-proBNP blood test.
“By identifying unrecognised heart failure in people with diabetes, we enable clinicians to initiate appropriate treatments sooner, ultimately improving patient outcomes and lives.”
News
UK government announces £6.3m fund to boost men’s health

The UK has launched a £6.3m men’s health fund to back local projects aimed at helping men and boys live longer, healthier lives.
The Men’s Health Community Fund is a partnership between the Department of Health and Social Care, Movember and People’s Health Trust.
The government is contributing £3m, while the two charities are more than doubling that to take the total to £6.3m.
Grants will support community projects reaching underserved men and boys aged 16 and over, particularly in the most disadvantaged areas and at key points in their lives such as becoming a father, losing a job or retiring.
Projects could include support for new fathers, activities for men facing loneliness and social isolation, services to help young men engage with the health system, and support for men in work, out of work and moving into retirement.
The programme will bring together voluntary, community and social enterprise organisations to test new ways of reaching men who are least likely to use traditional health services.
An evaluation funded through the National Institute for Health and Care Research will assess what works and help inform future policy and delivery.
Health and social care secretary Wes Streeting said: “Too many men across the country are living shorter, less healthy lives, particularly those in our most disadvantaged communities.
“This new partnership will help men get the support they need in the places they feel most comfortable, their communities, among people they trust.
“By working with expert charities and local organisations, we can reach the men who are too often missed by traditional services and help them take better care of their mental and physical health.”
“It is a key step in delivering our first ever Men’s Health Strategy and driving forward our ambition to halve the gap in healthy life expectancy between the richest and poorest areas.”
The Men’s Health Strategy sets out plans to tackle the physical and mental health challenges men and boys face.
Men can be less likely to seek help and more likely to suffer in silence, while higher rates of smoking, drinking, gambling and drug use are damaging men’s health and affecting families, workplaces and communities.
The government is also investing £3.6m over the next three years in suicide prevention projects for middle-aged men in local communities across areas of England where men are most at risk, many of which are also among the most deprived. Suicide is one of the biggest killers of men under 50, and three-quarters of all suicides are men.
The projects will aim to break down barriers middle-aged men face in seeking support, including stigma around asking for help and a lack of awareness of what is available and how to access it.
They will be co-designed with experts and men with lived experience of mental health crises and suicidal thoughts.